Healthcare organizations have long relied on legacy systems to manage critical operations. But as healthcare moves towards digital transformation, reliance on these outdated systems creates roadblocks, limiting hospitals’ ability to scale, innovate, and deliver high-quality patient care.
In this blog, let’s examine how legacy healthcare systems are impacting care delivery and how healthcare organizations can achieve application modernization.

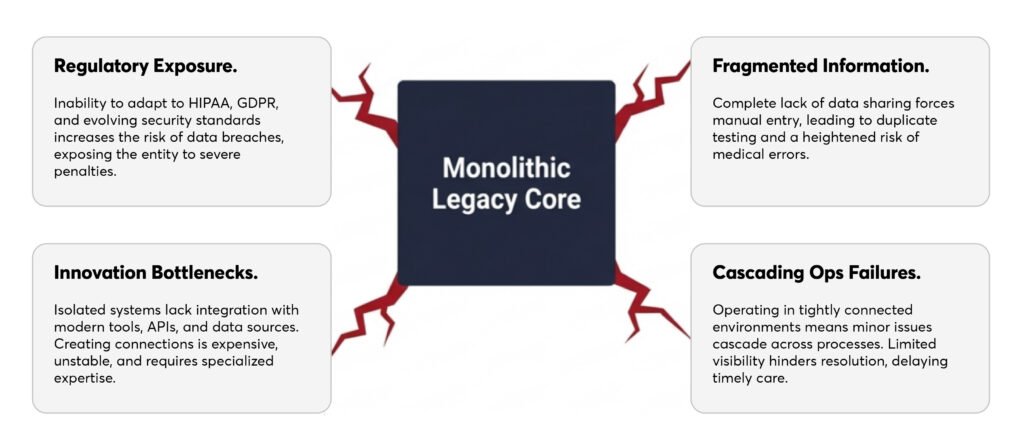
The top reasons why legacy systems fail to meet modern demands include:
Healthcare legacy systems must comply with HIPAA, GDPR, and data security standards. The HIPAA regulation requires covered entities and their business associates to protect electronic Protected Health Information (ePHI) that the organizations create, receive, maintain, or transmit.
If legacy systems do not comply with these regulations, the risk of data breaches increases, exposing organizations to penalties and sanctions.
Legacy systems struggle to communicate with modern Electronic Health Records (EHRs), telehealth platforms, lab systems, and medical devices. This lack of data sharing forces manual data entry that can lead to duplicate testing and increased risk of medical errors.
Legacy systems are isolated and monolithic; hence, they often struggle with integration. Connecting the outdated systems to modern tools, APIs, or data sources is complex and expensive, requiring specialized expertise and ongoing maintenance. The high cost, technical difficulty, and instability create a barrier to innovation, slow care delivery, and prevent organizations from fully leveraging digital transformation.
When operated in tightly connected environments, legacy healthcare systems can cause even minor issues to cascade across multiple processes. The limited visibility makes it difficult to quickly identify and resolve problems, leading to delays, inefficiencies, and increased operational strain, hindering timely care.
Incremental updates offer a less disruptive and more practical solution to complete system replacement. Phased modernization allows organizations to:
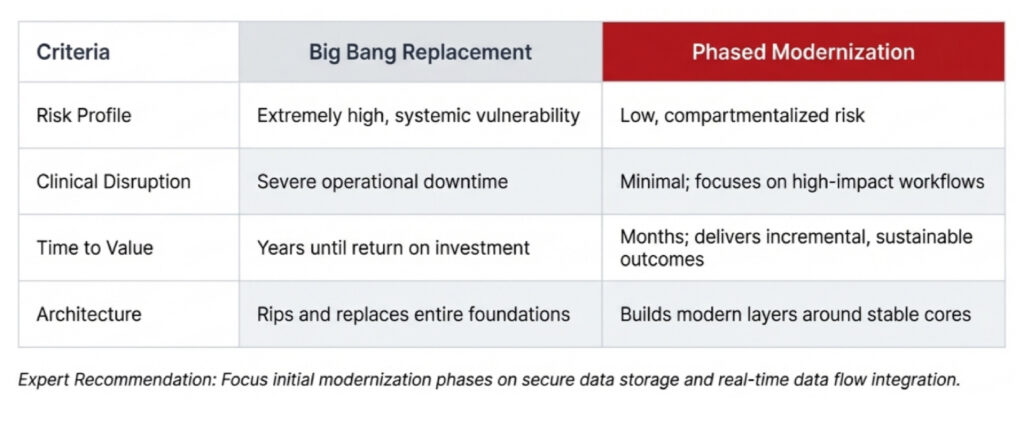
It is important to note that inefficiencies often stem from disconnected workflows, and integration challenges frequently reflect underlying process gaps.
Addressing these alongside modernization is what delivers real value, driving faster and more sustainable outcomes.
Leadership should no longer consider IT modernization as a “back-office” project but a core clinical and financial imperative.
InApp helps organizations take a structured and low-risk approach to modernization. The approach involves:

The first step toward modernization is understanding exactly where your vulnerabilities lie.
As you evaluate modernization, begin with a clear assessment of your current systems, risks, and priorities. Identifying high-impact opportunities early helps accelerate outcomes.
Connect with our team to explore where modernization can deliver the fastest and most meaningful impact.
A phased approach works best for modernizing legacy healthcare systems. Rather than replacing everything at once, focus on the most important areas first, update them gradually, and make sure all systems work well together.
The 7R framework is a strategy for evaluating legacy systems and determining the best modernization path. It includes options such as Retain, Retire, Rehost, Replatform, Refactor, Re-architect, and Replace.
Organizations need to include compliance at every step of modernization. This includes following data security and privacy standards such as HIPAA and GDPR, implementing access controls and encryption, maintaining audit trails, and ensuring systems are audit-ready.
The timeline varies depending on system complexity, organizational size, and modernization strategy. Phased approaches can deliver value in months, while full transformation may take several years.
To decide which systems to update first, organizations should consider factors such as business impact, risk, maintenance costs, and how well systems connect. Usually, the most important and riskiest systems should come first.